Osteoporosis is an old lady disease, right? Wrong.
I was diagnosed with osteoporosis aged 40 and for the past decade, bone health has been a hot topic for me. My goal is to assist others who have been diagnosed to seek help, make relevant lifestyle changes and make informed decisions around treatment and exercise – especially Pilates.
Osteoporosis and osteopenia can be a very stressful and scary diagnosis – many clients are told to wrap themselves in cotton wool, and to stop moving – but in many cases we need to keep moving, improving balance and building strength.
I’ve managed to reverse my diagnosis and I want others to know about the positive steps that they can take to improve their own bone health.

Over the years I have studied everything I can, read research papers, spoken to health care professionals, attended medical conferences, studied with Pilates industry leaders while being on my own quest to improve my bone health.
In April 2021 I was asked by Burrell Education to present at their women’s health conference for fitness professionals, Woman on Fire on Pilates for Bone Health, as well as Pilates for Mental Health – two subjects close to my own heart as a diagnosis of osteoporosis can really knock you for six mentally!
While the content of those presentations was aimed towards fitness professionals, I firmly believe this information should be available to our clients and to the general public too.
This article covers my own story as well as giving you an overview of Osteoporosis and how it is affects bone health and tips on lifestyle changes you can make after your diagnosis.
My Story
When I was diagnosed initially I was gobsmacked – I was young and it had been diagnosed by a chance health check. I had no symptoms or underlying conditions that I knew of. I was in shock and didn’t really believe it could actually happen or be happening to me.
Around the same time I’d just packed in a full time job and opened a Pilates studio. Not an ideal scenario when you’re told you should wrap yourself in cotton wool and about all the things in Pilates that you can no longer do in case you fracture.
Looking back, all of this took a toll not just physically but mentally on me too and it has now made me determined for my clients not to have the same experience.
Over time I realised it really was best not to continue to avoid the subject and so I started researching and figuring out what might be the best options for me to improve my bone health and get back to exercise safely.
- What would give me the best chances for improving my bone health?
- What effects does perimenopause and menopause have on bone health?
- What are my treatment options?
- What evidence based resources are out there?
- And most importantly, why do I have this diagnosis?
With consultation with my doctors, I took decisions around the treatments I chose, sought second opinions and changed my diet and other lifestyle factors as well as changing my exercise habits.
Unfortunately, at the time, many of the exercise changes I made were based on the “you have brittle bones, you could fracture at any time” guidance I received. Don’t do x, you better not do y. In fact it was all about what I couldn’t do. So I did less.
Not a good decision when our bodies rely on load to promote bone growth!
Why should you care about Bone Health?
The statistics speak for themselves.
- 1 in 2 women and 1 in 4 men over 50 years of age will suffer an osteoporosis-related hip, spine or wrist fracture during their lives.
- For women, the lifetime risk of a hip fracture is 1 in 6 versus a 1 in 9 risk of breast cancer
- 75% of all hip fractures occur in women.
- Increased mortality after hip fracture has been widely reported.
- The cumulative mortality after 1 year of a hip fracture occurrence ranges between 20 and 40%.
Currently, the majority of Pilates classes are still made up of women (though that is changing). We need to think about safety in our Pilates classes. Does a kyphotic 70 year old need to know how to do a Roll Over or Saw? There are many other more appropriate moves that this client could benefit from instead. We want to empower our clients to stay strong and capable and doing Pilates and other mindful movement practices throughout their lives.
Our Bones
Bone is living, dynamic tissue which is constantly being remodelled. Bone or osseous tissue is a hard tissue – a type of specialized connective tissue. Internally there is a honeycomb like structure which helps to give the bone rigidity, and this unique composition and design allows our bones to be relatively hard and strong, while remaining lightweight.
The process of bone remodelling happens when specialised cells called osteoclasts break down bone (resorption) and our osteoblasts work on new bone formation. As adults, approximately 10% of our skeletal mass is remodelled each year.
Our bones work together with our muscles and fascia to protect our vital organs and store minerals. They aid in our movement and form our red and white blood cells.
We reach peak bone mass by our mid 20s and after this our bone density begins to decline.

We have two main types of bone, trabecular and cortical.
Trabecular bone has an 80% faster metabolic turnover rate than cortical bone and is affected to a much greater degree by osteoporosis. However, it only makes up 20% of our total skeletal mass, cortical bone makes up the other 80%.
In the healthy skeleton these two cell types are continuously working in sync. Our thoracic spine, hips and wrists are areas where there is more trabecular bone and these are areas where we see more incidence of fractures.
What is Osteoporosis?
Osteoporosis was first recognised as a disease in 1994 by the World Health Organisation. They describe it as:-
“A systemic skeletal disease characterized by low bone mass and microarchitectural deterioration of bone tissue, with a consequent increase in bone fragility and susceptibility to fracture”.
So basically it’s a decrease in bone strength, which leads to an increased risk of fracture, though it is important a diagnosis does not guarantee a fracture.
Osteopenia is the early stages of Osteoporosis.
Assessment and Diagnosis
Bone density is assessed by DXA scan (Dual Energy X-ray Absorptiometry), which is like an X-Ray, and totally painless.
Measurements are taken of the lumbar vertebrae as well as the neck of the femur. They do not scan the thoracic spine or upper back as the bones of the rib cage would skew the results. However, if there is a diagnosis of osteoporosis in the areas scanned you can assume it is more than likely elsewhere also.
T-Scores
T-Scores are the measurement taken of the bone density and indicate the standard deviations below peak bone mass, relative to the age and sex-matched average.
Osteoporosis ranges are >-2.5 standard deviations below the avg value
Osteopenia ranges are from-1 to -2.4
with a further classification as follows
Mild Osteopenia -1 to -1.49
Moderate Osteopenia -1.5 to -1.9
Marked Osteopenia -2 to -2.49
For every 1-point standard deviation point we drop below the mean, the fracture risk doubles.
A DXA scan measures bone density but not bone quality though, so not everyone diagnosed with osteoporosis is guaranteed to have a fracture. Bone quality is measured by High Resolution Peripheral Quantitative Computed Tomography or pQCT scan.
Diagnosing Osteoporosis
Osteoporosis is a silent disease and is many times not diagnosed until someone has had a fragility fracture. A fragility fracture is where there is a fall from a standing height and a bone fractures – a low trauma break. It is beneficial to request a DXA scan if you have experienced a fragility fracture.
Some people, like myself, are diagnosed as part of a health screen. Or maybe there is a history of osteoporosis in the family and a DXA has been recommended.
Some symptoms of osteoporosis can include
- Fragility fracture
- Unexplained back pain and muscle spasms
- Height loss
- A very rounded upper back spine or change in posture
- Breaking a wrist during a fall from standing height
Something to note – osteoporosis doesn’t affect the healing process of bone. So if you do break a bone, it can heal as normal over the course of between six and 12 weeks.
Types of Osteoporosis
Both women and men are affected, though osteoporosis is more prevalent in women.
Type 1 Postmenopausal, Most Common
- Estrogen deficiency due to menopause
- 2-3% bone loss for about 10 years.
- Increased rate of bone resorption as we age
Type 2 Senile 70+
- More sedentary
- Possible long term calcium deficiency
- Vitamin D levels generally low
Secondary Osteoporosis
There can be many reasons for secondary osteoporosis, some of which are listed below
- Predisposing medical problems or disease
- Long term use of certain medications such as steroids or anti-seizure meds
- Diet and nutrition issues
- Some cancer treatments
- Coeliac Disease and gluten intolerances that affect our ability to absorb the nutrients we eat
Building Bone
Obviously the best plan is to lay down as much bone as we can in our younger years – running, jumping, dancing and skipping are all great ways to get kids moving.
Bone is continually deposited and resorbed or reshaped in response to the stresses we put on it.
It is mechanosensitive in that if we load it, it will strengthen – form follows function according to Woolf’s Law. So we need to move more, and add strength training to our exercise programs.
Specificity
Where we load as much as how we load it is important. We need site specific programming especially in the spine, wrists, hips – as well as body-wide multi dimensional movement for joint health and mobility as well as bone strength. the dosage may differ though between a frail, elderly adult to an active pre-menopausal woman.
Lifestyle Factors
There are many reasons for an osteoporosis diagnosis that we can’t do anything about bu there ARE changes we can make to our lifestyles that can help address bone density issues.
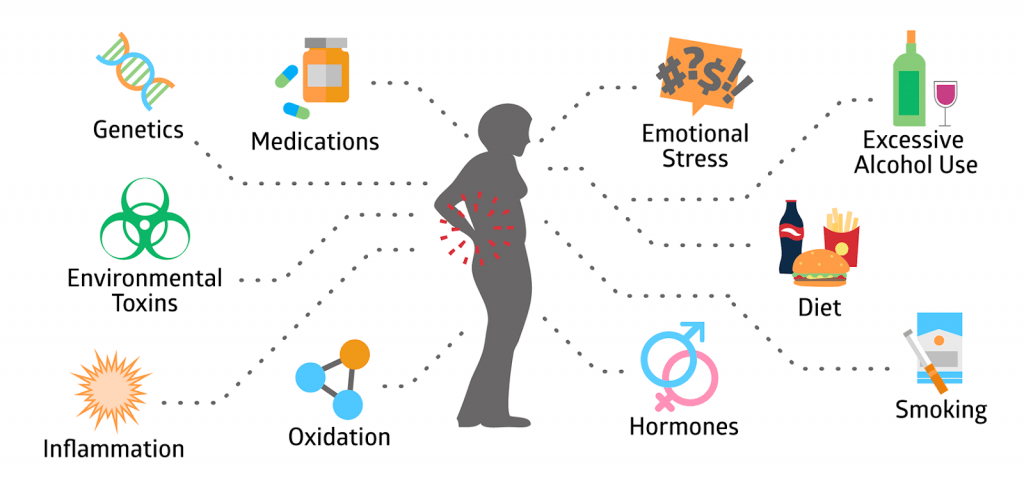
- Improving our diet & nutrition and including more plant based options
- Ensuring we get plenty of calcium and vitamin D is essential.
- Increasing calcium intake in diet (there are many calcium rich foods including dairy)
- Reducing alcohol
- Stopping smoking
- Reducing stress levels
- Improving Sleep
- Increasing weight bearing exercise
Medication
Medication is available for those who need it. Deciding to go down this route is an individual choice that is made based that person’s particular history and what their fracture risk is. Researching the options out there with your health care professional is critical, as well as a good understanding of why you have the disease in the first place.
Biphosphonates have been around since the 1960’s, and newer drugs such as Prolia have also entered the marketplace more recently.
In my case when I was first diagnosed I had a recommendation of HRT, but unfortunately for me at the time the press and media were full of stark and incorrect warnings about the increased cancer and heart risks associated with hormone replacement therapy – despite strong evidence provided in the WHI (Women’s Health Initiative) and previous studies that estrogen is highly effective in preventing fractures. Unfortunately based on this, I chose not to take HRT until more recently.
The guidance is now that HRT is in fact very beneficial and should be prescribed for more women for it’s health benefits. Read this article by Dr Louise Newsome for more information on the benefits of HRT.
How Can Pilates Help?
“Ideal alignment facilitates optimal movement”
– Shirley Sahrmann
Strong legs and extensors, an upright posture, good balance and alignment and awareness are key to staying upright and fracture free. Sounds just like Pilates right?
As ever, we want to help our client’s improve their body awareness – both proprioception and interoception to improve kinesthetic awareness overall. We also need to teach for transfer outside the studio too – so there’s a good understanding of how to lift heavy weights (so important!) or garden safely without putting themselves at more risk of fracture. We can follow Pilates principles, with intelligent modifications and assists where needed.
According to the Royal Osteoporosis Society, it is OK to continue as you were if you have been doing Pilates for many years and have no history of fracture – after all, we need to be able to flex our spines as part of our everyday movements. But thinking intelligently about range of movement, compressive forces down into the vulnerable points in the vertebrae and uncontrolled movements as part of your programming is essential. Do you really need Short Spine or Roll Over in your practice? A modified Pilates practice can still be challenging and enjoyable!
You can of course make these choices for yourself if you have had a diagnosis – but for teachers it is imperative to educate your clients on the risks.
That said, maybe Jack Knife or Long Spine might be off the table, but with skilful teaching we can add other repertoire without our clients feeling negative about the moves they can no longer do. Of course, if there has been a fracture previously, it is imperative that additional precautions should be taken.
Staying positive, upbeat and challenging them within their ability to keep good alignment with progressive loading and resistance with springs in apparatus is ideal support for clients to add load, safely.
Pilates has many benefits for osteoporosis and osteopenia clients –
- Improves balance to reduce fall risk
- Focus and flow can help with stress
- Builds strength
- Bone strengthening
- Improves joint mobility
- Can be site specific as well as a full body workout
- Promotes awareness in other activities
A Modified Pilates Practice
There is no one size fits all approach to working with osteoporotic clients. Some will be more frail than others – some will be fit and strong, others need to work with in an upright position without ever getting down to the mat (the WundaChair comes into it’s own here). An individualised program can really help these clients to build their strength and flexibility, safely.
As teachers we need to add more standing and balance work in our sessions to help reduce the risk of falls and to improve arm and leg strength. Apparatus such as the Reformer and Cadillac are wonderful tools to provide support and challenge for our clients as well as a modified matwork practice. As the Pilates apparatus is inherently designed to be unstable, spotting clients and ensuring safety while on the equipment is key which is why it’s so important to work with a qualified, knowledgeable teacher. The small adjustments and modifications given by a trained eye can make all the difference!
Studies show strengthening of major appendicular muscles decreases fragility so adding more leg and arm work to our programs is key – we lose 1% of our leg strength per year after age 50! Arm and leg work on the Chair, Cadillac and Reformer are great additions to any program. As previously mentioned the dosage may need to be adjusted for each individual.
Working in extension is key for these clients, to open up the front line of the body and to strengthen the back lines. The Spine Corrector enables us to work from extension to neutral and avoid any compressive loads on the anterior portion of the vertebrae while providing support and comfort too.
There is a very famous study back in 1984 by Sinaki & Mikkelson, where they tested four separate groups of subjects with osteoporosis.
Group 1 EXTENSION
16% had another wedge or compression fracture
Group 2 FLEXION
89% had another wedge or compression fracture
Group 3 EXT + FLEX
53% had another wedge or compression fracture
Group 4 NO EXERCISE
67% had another wedge or compression fracture
As part of this study, they also found that the thoracic vertebrae T7, T8 and T6 (in that order) are the most prone to fracture. Working in a site specific manner with appropriate modifications to range of movement, additional props etc is necessary for osteoporotic clients.
Getting Started with Pilates
It is good practice to request clearance from a medical practitioner when working with osteoporosis and osteopenia. A detailed screening questionnaire should be completed in advance of your first session.
This should include details on any history of fracture, include your T-scores. This can be requested from your doctor – or from the hospital / clinic at the time of your DXA scan.
Your teacher will review and will give an initial indication if their Pilates program will be a good fit.
During the subsequent initial assessment you can discuss the completed health form and begin your assessment with your teacher. These could include:-
- Can you get up and down off the floor easily?
- Sit to stand test
- Can you stand without using your hands?
- Do your knees draw together as you stand?
- How many times can you sit to stand in 15 seconds?
- Occiput to wall distance (measures forward head posture and spinal angle)
- Functional reach test – 10” or more is normal – fear of bringing head in front of body
- Ribs to pelvis distance 2-4 fingers is normal
- TUG – Timed Get up and Go test
- Walk 3 metres, turn around, walk back and sit down. 10-20 seconds minimal fall risk. More than 30 seconds indicates a fall risk
Progressing your Practice
In some cases it is possible to reverse a diagnosis of osteoporosis back to osteopenia and back to normal ranges if lifestyle changes are made, bone strenghtening exercise is increased and with appropriate medications if needed – but each and every individual differs.
If you or your client has been diagnosed with osteoporosis, a regular DXA will be recommended by your health care professional (every 1-2 years) so be sure to check in with your T-Scores regularly.
Once a client’s ranges are back to normal you can add back more of the Pilates repertoire, but if there is a history of spinal fracture a modified practice will continue to be needed.
Resources
- Royal Osteoporosis Society
- Irish Osteoporosis Society
- British Menopause Society
- The Menopause Doctor
- Mayo Clinic
- NHS
- Wellness Warrior
About Me
I’ve been a Pilates fan since the late ’90s, and decided to certify as a teacher in 2005. Since then I’ve been hooked and have taught hundreds of clients thousands of hours of Pilates and movement sessions.
After many years double jobbing in both the Pilates and IT world, I founded Live & Breathe Pilates in 2008 and I finally took the plunge into full time teaching in 2012 when I opened a purpose built Pilates studio in Dublin city centre. Since then I have the built the studio into a thriving community hub with a team of ten teachers.
My passion is teaching people how and why Pilates and myofascial movement can help reduce pain, improve flexibility and build their strength, enabling them to improve their game or get back to doing the things they love. I have taught many thousands of hours of Pilates and mindful movement to clients of all abilities – from octogenarians to professional athletes.
Our studio is also a centre of excellence for Pilates training and continuing education for movement teachers worldwide. The courses I have curated attract teachers from all over the globe – South Korea, Australia, Israel, US, UK and Europe – and I continue to teach classes to a worldwide audience through our online offerings.
I also mentor for Pilates teachers in training and provide ongoing movement classes and workshops for teachers. As a mentor, imparting evidence based knowledge to the next generation of teachers has it’s own rewards as I see the Pilates community in Ireland grow.
I have presented at international conferences, providing workshops on topics such as Pilates for Spinal Care, Pilates for the Postnatal Client and Pilates for Mental Health as well as teaching regular workshops and courses for teachers and clients alike.
I love to learn and can consistently be found nerding out on anatomy, fascia and movement and talking the ear off anyone who’ll listen about the never ending connections between mind and body.



